A Voucher for Psychological Well-Being? Researchers and Practitioners Discuss Lasting Well-Being Benefits from a One-Time Voucher Program
By Erin Kelley, Leslie Roberts, Emily Sloane, John Quattrochi, and Pieter Ventevogel
There are currently 244 million people worldwide affected by humanitarian crises, including 84 million who have been forcibly displaced. The displacement crisis in countries bordering Ukraine is a reminder of the many ongoing displacement crises which also need the world's urgent attention. To focus on solutions, we look back on a lively discussion and debate between a group of researchers and practitioners discussing a straightforward one-time program for displaced and vulnerable people that had lasting impacts a year later. What followed was a discussion that we think has implications for future research, so while you can watch the video here, we present here a very brief summary of the findings and discussion points, which might serve as a jumping-off point for new studies.
Professor John Quattrochi presented his research, done with Ghislain Bisimwa, Peter Van der Windt, and Maarten Voors, in the eastern Democratic Republic of Congo (DRC). While studies abound on the benefits of direct economic support to the poor around the world, it is much more difficult to run such studies settings in crisis-affected or similar settings, such as with displaced populations. But people in conflict settings are much more vulnerable to psychological distress and trauma. Serious psychological disorders like depression and Post-Traumatic Stress Disorder (PTSD) are three times greater in conflict settings, and conflict creates a fivefold increase in years lost to disability due to depression and PTSD.
The research, conducted with the NGOs Mercy Corps, Solidarités International, Norwegian Refugee Council, and Danish Refugee Council, looked at whether providing straightforward material support vouchers to buy household items like mattresses, tarps, and cooking implements, helped with physical and psychological health, social cohesion, and resilience. For the study, an existing program for internally displaced people in the DRC was extended to a randomly selected group of vulnerable families who would not have otherwise qualified for it (976 households were enrolled in the study, half of whom received the vouchers, and half continued as normal).
The study found:
- At baseline, one-third of respondents met the criteria for clinically-significant depression or anxiety.
- About six weeks after the transfer of the vouchers, there were strong improvements in psychological well-being for those who received the vouchers. A year later the effects were weaker but still evident (Figures 1-3).
- No evidence of an impact on social cohesion, suggesting that targeting some households in the village but not others did not undermine local community relations.
- No overall effect on economic resilience, but household assets and dietary diversity improved, suggesting a mechanism by which economic assistance can improve psychological well-being.
- No effect on child health, suggesting health challenges (malaria, diarrhea, etc.) are too persistent to change using this level and mode of aid disbursements.
Note: the discussion continues following the figures below.
Figure 1. Life satisfaction in treatment and control groups at baseline, six weeks, and one year
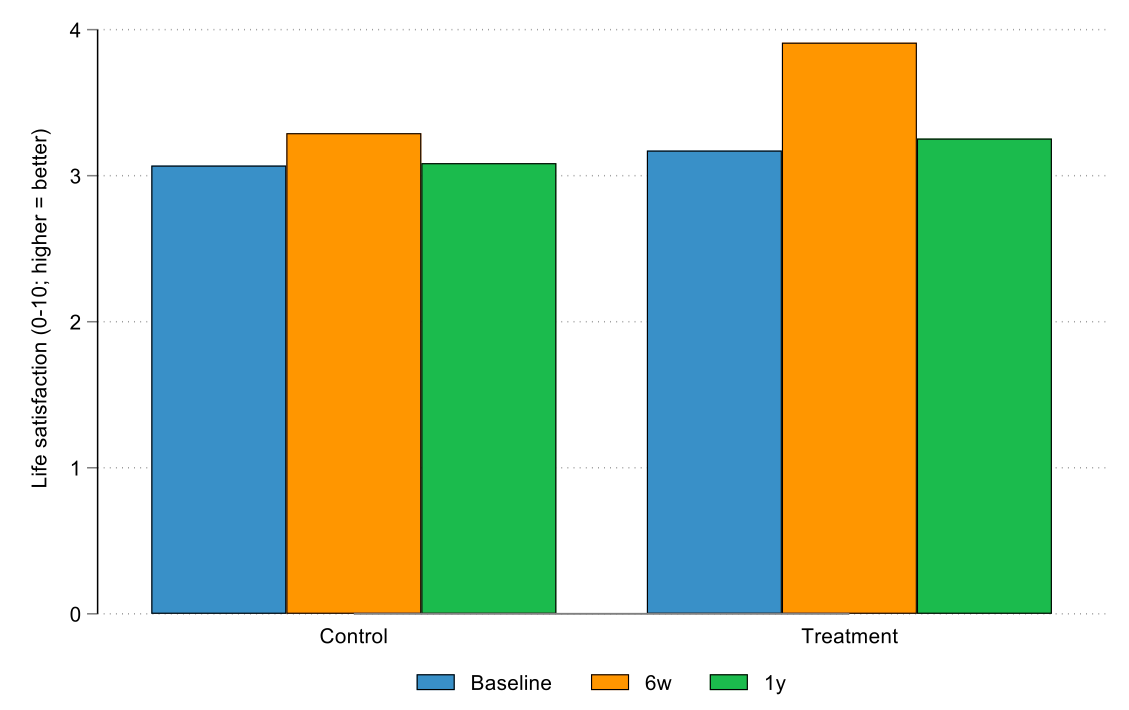
Figure 2. Subjective well-being in treatment and control groups at baseline, six weeks, and one year
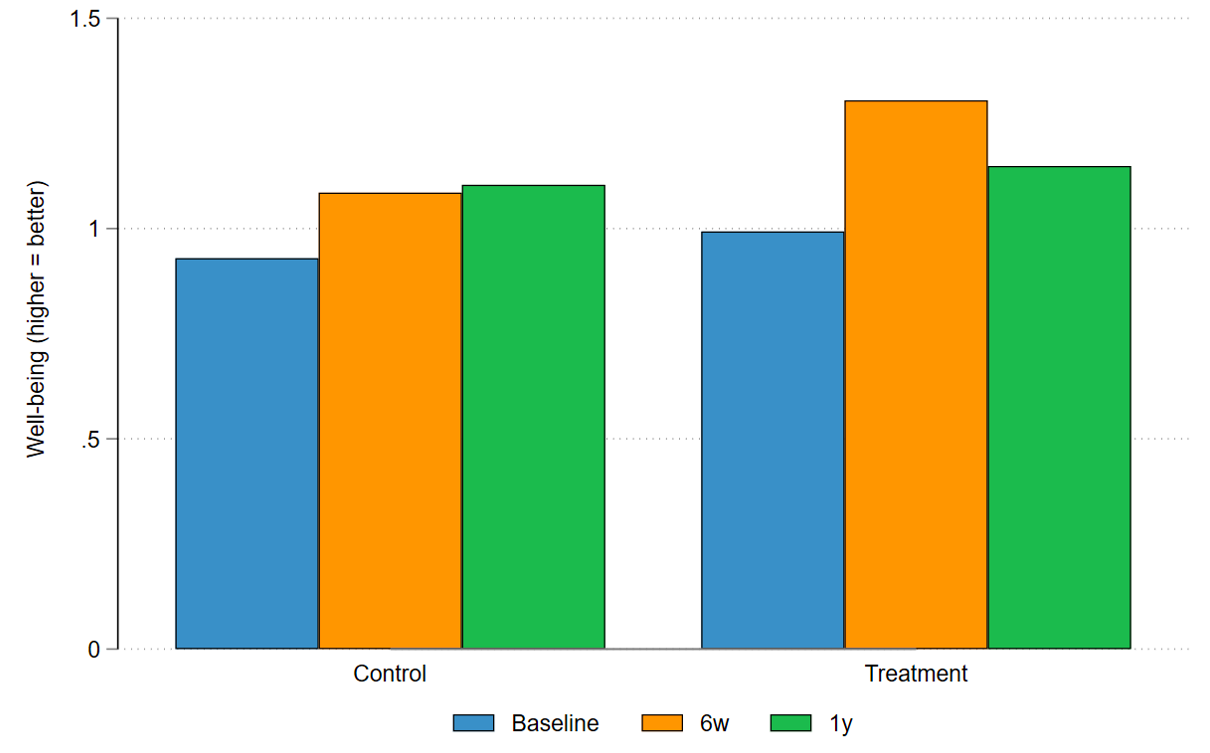
Figure 3. Depression/anxiety in treatment and control groups at baseline, six weeks, and one year
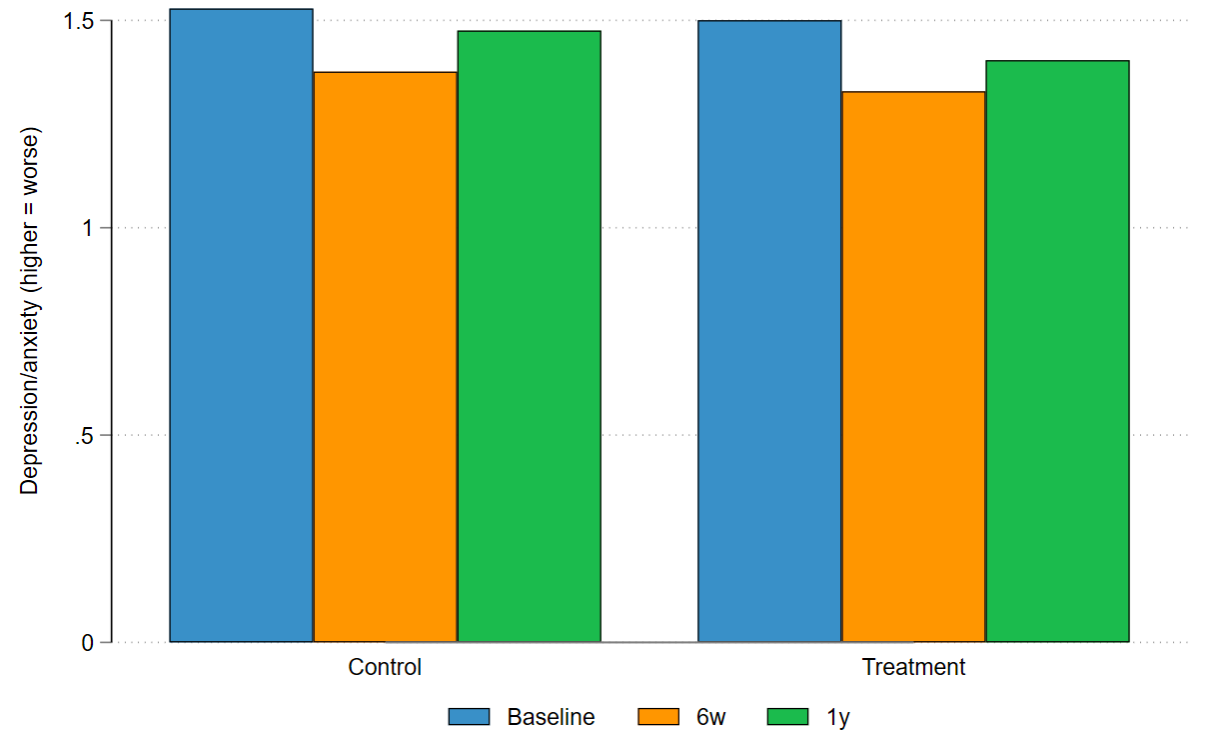
Figure 4. Average effects of vouchers (lower values mean improvements, bars show 95% confidence intervals)
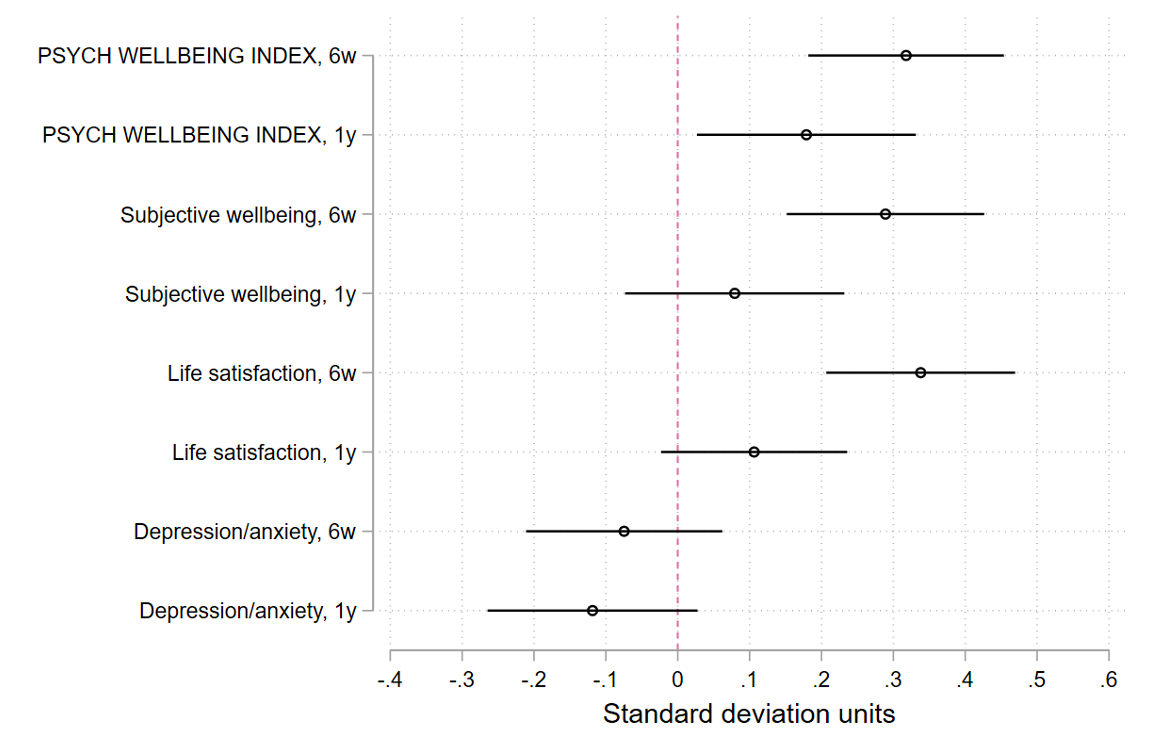
Figure 5. Average treatment effect of vouchers at six weeks and one year after voucher distribution (bars show 95% confidence intervals)
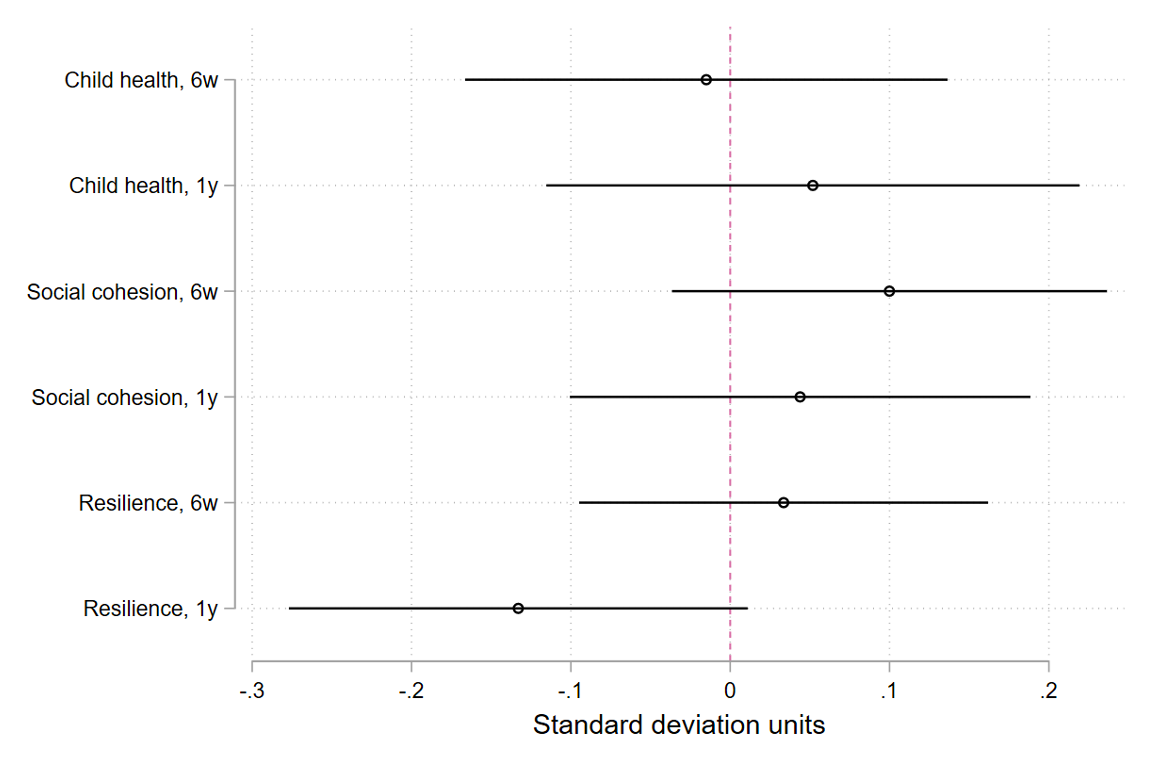
Professor Leslie Roberts, of Columbia University, made three points. First, the mental health burden is the main driver of disability-adjusted life year loss in conflict settings. The big difference from other drivers is that we do not have treatments for mental illness that are as effective as treatments for, say, malaria or diarrhea. Second, unlike many other mental health studies, this study did not select the most mentally troubled participants. Therefore, the results may be more generalizable.
Third, cash and cash vouchers have multiple effects that vary across settings, including, in some cases, improved nutrition among children. In some aid programs, vitamin A has become a standard part of many packages because it makes a big difference in some places. While it is hard to know in advance in which settings it will help and exactly how much because there are no downsides to it, it has become easier to give to everybody. It’s possible that programs like this which have varied but broad benefits will have the potential to be the new Vitamin A.
World Bank economist, Erin Kelley suggested further probing the mechanisms behind the observed effects—such as whether the benefit comes from less pressure to meet daily material needs versus perceptions of being better off than people around them. Drawing on her own work in Bangladesh she also pointed to the difficulty of measuring subjective factors such as mental health and well-being with instruments validated for local use and pointed out how the field would benefit from a publicly available database of instruments on psycho-social wellbeing, along with establishing best practices to minimize social desirability bias and other pressures for respondents to answer in a particular way. Lastly, Dr. Kelley proposed additional research investigating the relative benefits of vouchers versus cash; mental health programs versus cash/vouchers; and, cash for work versus unconditional cash/vouchers.
Emily Sloane, Economic Recovery and Development Technical Advisor at the International Rescue Committee, noted that mental health and psychosocial support is under-resourced, in part because of insufficient evidence. There is also some tension between sectors: Health teams are often unwilling to move away from direct service delivery, and cash/food security actors are often wary of expectations that basic needs-focused interventions—such as the NFI vouchers featured in the research—should achieve non-basic needs outcomes. The standard understanding, based on a fair amount of research on non-basic needs outcomes, is that cash and voucher assistance can often help to enhance other outcomes but is best used in combination with other, more sectoral, interventions. Emily noted that the study’s findings on longer-term impacts of cash/vouchers were a valuable contribution to the evidence base. She also echoed Erin’s call for a better understanding of mechanisms and pointed out that we don’t know how cash or vouchers for basic needs actually contribute to the achievement of other outcomes—such as improved mental health—in practice, which makes it important to understand the pathways through which they work in order to advocate for better program design.
Pieter Ventevogel, psychiatrist and Senior Mental Health & Psychosocial Support Officer, UNHCR, put this study in the context of mental-health-focused interventions. He noted the important difference between psychological distress and mental disorders. The former is transient and very common in humanitarian settings, but that’s different from the latter, which are severe and impact social and occupational functioning. Once mental disorders reach a high level of severity, they may be unresponsive to material assistance and require specialized psychiatric care. Furthermore, there is a strong evidence base growing just in the past few years for scalable psychological interventions that only require 5-12 sessions, but we shouldn’t be disheartened to see effects fade over time, the same would be true for a malaria one-time intervention a year later.
As a clinician though, Pieter noted the practitioners’ reminder to researchers that statistical significance does not necessarily imply clinical relevance. Echoing previous commentators he also hypothesized about mechanisms—perhaps an increased sense of agency or self-efficacy may be driving the improvements in psychological well-being, but added that we shouldn’t see cash or vouchers as a non-mental health program. From where he sits, traditional clinical services are a relatively small part of mental health aid, which is built on a much larger base of programs that strengthen everyday community support and basic services, where this program can be squarely positioned. Pieter concluded by posing multiple questions for future research: will cash-based interventions generate similar benefits in other settings? What modality is best? Who benefits most? Are psychological interventions complementary to cash (i.e. are there synergistic effects)? How cost-effective is cash?
Many of the questions raised we think can help chart future research agendas in the rapidly growing areas of cash/material support and mental health research. IPA has several studies ongoing in these areas and would love to hear from researchers interested in the topics.